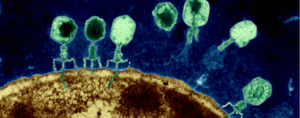
 Some researchers are now testing to see if phage therapy could be a possible treatment for some conditions, such as chronic sinusitis and wound infections. Phage therapy, which uses bacteriophages, was neglected for decades (except for Russia and the Republic of Georgia), but their use is again being studied as an alternative to antibiotics. A bacteriophage is a virus that lives within a bacterium, replicating itself, and eventually destroys the bacteria. The term is from "bacteria" and the Greek "phagein" which means to devour, so think of them as "bacteria eaters". Phages only attack specific types of bacteria (they are "bacterium specific"), so they’re unlikely to harm the normal microbiome (community of microbes) or any human cells.
Some researchers are now testing to see if phage therapy could be a possible treatment for some conditions, such as chronic sinusitis and wound infections. Phage therapy, which uses bacteriophages, was neglected for decades (except for Russia and the Republic of Georgia), but their use is again being studied as an alternative to antibiotics. A bacteriophage is a virus that lives within a bacterium, replicating itself, and eventually destroys the bacteria. The term is from "bacteria" and the Greek "phagein" which means to devour, so think of them as "bacteria eaters". Phages only attack specific types of bacteria (they are "bacterium specific"), so they’re unlikely to harm the normal microbiome (community of microbes) or any human cells.
I've been posting about the beneficial bacteria Lactobacillus sakei that treats chronic sinusitis, as well as some other probiotic (beneficial) bacteria that people have reported success with (see The One Probiotic That Treats Sinusitis). Most people contacting me or commenting have reported success with L. sakei products, but there is a group for whom L. sakei and other probiotics haven't helped. Why? And what can be done? Perhaps their sinuses are missing still unknown "keystone" species (very important microbial species for health). Or perhaps they have bacterial biofilms that even Lactobacillus species that are viewed as anti-biofilm cannot overcome. Perhaps phage therapy might help these people?
Phage therapy is currently being tested by researchers in the treatment of chronic sinusitis in Australia. The video Antibiotic Resistance discusses phage therapy for sinusitis starting at 23:30. Looks promising.
And a write-up about the sinusitis phage therapy research from the Australian newspaper The Sydney Morning Herald: Medicine turns to bacteriophage therapy to beat superbugs
An arcane therapy for bacterial infections that dwelled behind the Iron Curtain for decades is making a comeback in Western medicine as a potential white knight against superbugs. Phage therapy involves infecting patients with viruses known as bacteriophages, which are the natural predators of bacteria, to kill the germs that antibiotics cannot. ...continue reading "Phage Therapy May Help Sinusitis Sufferers"
