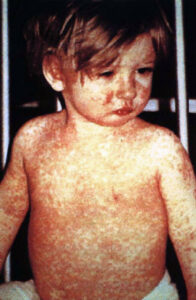
In the year 2000 the United States had a "measles elimination status" meaning measles had been eliminated in the US, but that's now over. So far in 2026 there have been 1671 measles infections, according to the Centers for Disease Control and Prevention (CDC). In this past week alone there were almost 100 new cases, almost all in Utah.
Measles infections (which are bad enough) can have very serious complications, including death. According to the CDC these include severe ear infections (leading to hearing loss), severe diarrhea, pneumonia (can cause death), encephalitis (brain swelling) resulting in permanent brain damage, complications during pregnancy, and even the rare fatal condition subacute sclerosing panencephalitis (SSPE) that can occur years later (typically 4 to 8 years later).
Scary facts about measles (from the CDC): about 1 in 5 unvaccinated people in the US who get measles is hospitalized, about 1 child out of every 1000 who get measles will develop encephalitis (brain swelling), and nearly 1 to 3 of every 1000 children who become infected with measles will die from respiratory and neurologic complications.
Yeah, the measles vaccine works, but only if you get vaccinated. By the way, a measles infection is especially deadly to babies because they are still too young to get vaccinated - which normally occurs at 12 to 15 months of age,
Excerpts from rom CIDRAP (Center for Infectious Disease Research and Policy): US nears 1,700 measles cases, with 73 new infections in Utah
US measles cases climbed by almost 100 in the past week, reaching 1,671 infections, the Centers for Disease Control and Prevention (CDC) said today in its weekly update. The vast majority of the 96 new cases are in Utah. ...continue reading "Measles Can Be Deadly"

 Not only humans and many foods (e.g., fruits) have microbiomes - the community of bacteria, viruses, archaea, and fungi living on and in the organism.
Not only humans and many foods (e.g., fruits) have microbiomes - the community of bacteria, viruses, archaea, and fungi living on and in the organism.  There has been discussion over the years regarding mouthwash - what are the harms and benefits? Does using
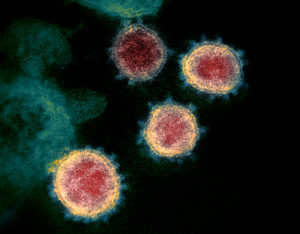
There has been discussion over the years regarding mouthwash - what are the harms and benefits? Does using  Millions of us have had a least one COVID infection. Many suffered a loss of smell during the infection. A recent
Millions of us have had a least one COVID infection. Many suffered a loss of smell during the infection. A recent 
 It is still unknown whether probiotic supplementation would help these conditions because the studies are not yet done. But researchers do suggest eating an anti-inflammatory diet - which means a diet rich in fruits, vegetables, whole grains, legumes (includes beans), fish, seeds, nuts, and olive oil. This kind of diet has lots of fiber to feed and support beneficial bacteria.
It is still unknown whether probiotic supplementation would help these conditions because the studies are not yet done. But researchers do suggest eating an anti-inflammatory diet - which means a diet rich in fruits, vegetables, whole grains, legumes (includes beans), fish, seeds, nuts, and olive oil. This kind of diet has lots of fiber to feed and support beneficial bacteria. Millions of pounds of pesticides are used each year in the US: on farms, in buildings and homes, on lawns, in pet flea and tick products - basically everywhere. And so the pesticides eventually wind up in us - from the foods we eat, the water we drink, the air we breathe (when pesticides drift during applications or when used indoors), and the treated lawns and ground we walk on.
Millions of pounds of pesticides are used each year in the US: on farms, in buildings and homes, on lawns, in pet flea and tick products - basically everywhere. And so the pesticides eventually wind up in us - from the foods we eat, the water we drink, the air we breathe (when pesticides drift during applications or when used indoors), and the treated lawns and ground we walk on. Exercise helps fight cancer. Wow! What a headline. But is it true?
Exercise helps fight cancer. Wow! What a headline. But is it true?
 Over the past decade there has been as increasing amount of research suggesting that the herpes virus (cold sores!) is implicated in the development of Alzheimer's disease. (
Over the past decade there has been as increasing amount of research suggesting that the herpes virus (cold sores!) is implicated in the development of Alzheimer's disease. (