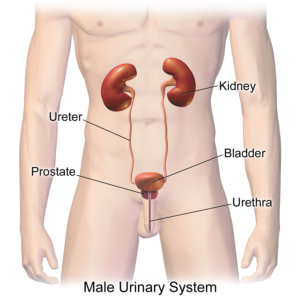
Chronic kidney disease (CKD) is a growing problem globally, especially in aging populations. As people age, their kidney function declines - and this is a normal part of aging. A recent study found that physical activity slows this kidney function decline.
The study followed healthy individuals (aged 50 to 64 years at the start), who had varying physical activity levels, over an 11 year period. The researchers found that there is a dose response effect from physical activity - more active persons had a slower annual kidney function decline, as well as a much lower risk of accelerated kidney function decline.
The slowest level of kidney decline was in persons who were physically active almost every day (at least 5 days a week) and who engaged in more intense exercise. Note that physical activity is not just doing exercises - it's physical activity of all sorts. Yes, walking counts.
 The researchers viewed physical activity as having reno-protective effects - in both the general population and in persons with CKD. This is because it lowers the risk of developing CKD, but it also slows kidney function decline. By the way, other studies have also found physical activity or exercise beneficial in slowing down the kidney function decline that occurs with aging.
The researchers viewed physical activity as having reno-protective effects - in both the general population and in persons with CKD. This is because it lowers the risk of developing CKD, but it also slows kidney function decline. By the way, other studies have also found physical activity or exercise beneficial in slowing down the kidney function decline that occurs with aging.
From Medscape: Physical Activity May Slow Kidney Function Decline
Increased physical activity was associated with a substantially lower risk for kidney function decline, with the strongest effects seen with higher frequencies and intensities of activity, according to a new longitudinal study. ...continue reading "Physical Activity Slows Down Kidney Function Decline That Occurs With Aging"

 There has been lots of research in the past decade over the benefits of eating a diet rich in fruits, vegetables, whole grains, nuts, and legumes, especially a Mediterranean style diet. Health benefits include lowering chronic inflammation and a lower incidence of a number of chronic diseases, including type 2 diabetes.
There has been lots of research in the past decade over the benefits of eating a diet rich in fruits, vegetables, whole grains, nuts, and legumes, especially a Mediterranean style diet. Health benefits include lowering chronic inflammation and a lower incidence of a number of chronic diseases, including type 2 diabetes. As people age, they frequently start wondering what they can do to prevent memory and thinking problems, and especially dementia. The good news is that several large studies found that there are a number of lifestyle changes that one can do to have a healthier (memory! thinking!) brain in later years. Even if you are already in your 60s and 70s.
As people age, they frequently start wondering what they can do to prevent memory and thinking problems, and especially dementia. The good news is that several large studies found that there are a number of lifestyle changes that one can do to have a healthier (memory! thinking!) brain in later years. Even if you are already in your 60s and 70s. Exercise helps fight cancer. Wow! What a headline. But is it true?
Exercise helps fight cancer. Wow! What a headline. But is it true?
 Exercise boosts brain function at all ages. This means that for both young and old, it is worth it to get out and engage in physical activity.
Exercise boosts brain function at all ages. This means that for both young and old, it is worth it to get out and engage in physical activity.