 Another study finding overdiagnosis (diagnosing something that isn't likely to cause problems) and misdiagnosis (diagnosing something that isn't there) which leads to overtreatment (unnecessary treatment) - this time of asthma in adults. A new study found that as many as 1 in 3 adults diagnosed with asthma may not actually have the disease. Was this due to spontaneous remission or to initial misdiagnosis? After all, many other diseases mimic the symptoms of asthma, and there is no test that can diagnose asthma with 100% accuracy. The study authors thought that of the 33% without asthma - that many of the adults had been originally misdiagnosed, while others had gone into remission. Excerpts from the thought-provoking site Health News Review:
Another study finding overdiagnosis (diagnosing something that isn't likely to cause problems) and misdiagnosis (diagnosing something that isn't there) which leads to overtreatment (unnecessary treatment) - this time of asthma in adults. A new study found that as many as 1 in 3 adults diagnosed with asthma may not actually have the disease. Was this due to spontaneous remission or to initial misdiagnosis? After all, many other diseases mimic the symptoms of asthma, and there is no test that can diagnose asthma with 100% accuracy. The study authors thought that of the 33% without asthma - that many of the adults had been originally misdiagnosed, while others had gone into remission. Excerpts from the thought-provoking site Health News Review:
Is it asthma? Many diagnosed with condition receiving unnecessary or incorrect treatment
As many as 1 in 3 adults diagnosed with asthma may not actually have the disease, according to new research published in the Journal of the American Medical Association (JAMA). Canadian researchers evaluated 613 patients with physician-diagnosed asthma and found that 203 participants (33%) most likely did not have the disease. After an additional 12 months of follow-up of this latter group, 181 subjects (30%) continued to exhibit no clinical or laboratory evidence of asthma.
This study, and its accompanying editorials, hit on a theme we’ve often raised with regard to cancer and many other chronic diseases: overdiagnosis leading to overtreatment. But it also raises the specter of misdiagnosis from the get-go, which can lead to erroneously treating a condition that isn’t there. The Canadian results may also confuse many of us who have grown accustomed to news stories warning us that asthma is on the rise. So which is it? More asthma which needs more aggressive treatment or less asthma warning against overtreatment?
“I think asthma is both overdiagnosed and underdiagnosed,” says Dr. Nancy Ott, an allergy and immunology specialist in practice for 28 years. “We don’t have a specific test that is definitive for asthma, and the diagnosis is nuanced. You need to look at the symptoms, the patient’s history, their family history, and the objective tests collectively. And I think we need to be much more strict in what constitutes asthma because the symptoms alone overlap with so many other conditions.”
This is not a message we hear nearly enough in news stories: the diagnosis of asthma, although common, is anything but cut-and-dried. In outpatient clinics – where most asthma is diagnosed – time pressures can lead to incomplete evaluations, which lead to misdiagnoses (which, by the way, includes over-, under-, and no diagnoses), and this can ultimately lead to patients suffering physically, emotionally and financially.
“We think that a large proportion of them had been misdiagnosed in the first place and another proportion that (was) a bit smaller had actually gone into remission, their asthma was no longer active,” said principal investigator Dr. Shawn Aaron, head of respirology at the University of Ottawa. Medical textbooks say about six per cent of people with asthma go into remission over a 10-year period, said Aaron. “But we found at least 20 per cent had gone into remission.” However, “one of the main messages I want to get across is that some people are being misdiagnosed because they’re not being properly investigated to begin with,” he said from Ottawa.
Which brings up an important point: the symptoms of asthma overlap with several other diseases. In the Canadian study, 12 people, or 2 percent of the participants, had serious conditions other than asthma, like heart disease and pulmonary hypertension. Others had problems such as hyperventilation from panic attacks, and gastroesophageal reflux (GERD). These latter two conditions frequently mimic asthma. As does vocal cord dysfunction. Suffice to say that if you were to take each of the classic symptoms of asthma individually, the list of diseases associated with that symptom is well over a dozen.

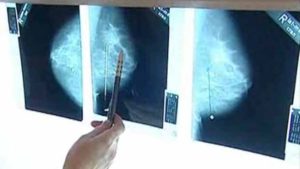 Another large study looking at screening mammograms for breast cancer has raised the issue of overdiagnosis and overtreatment once again. The purpose of mammography screening is to find cancer when it is small and so prevent cancer from growing and becoming advanced cancer. However, the researchers did not find this - there was a major increase in finding small cancers (the kind that may grow so slowly as to never cause any problems or that may even regress), but the rate of advanced cancers stayed the same.
Another large study looking at screening mammograms for breast cancer has raised the issue of overdiagnosis and overtreatment once again. The purpose of mammography screening is to find cancer when it is small and so prevent cancer from growing and becoming advanced cancer. However, the researchers did not find this - there was a major increase in finding small cancers (the kind that may grow so slowly as to never cause any problems or that may even regress), but the rate of advanced cancers stayed the same. The problem of overdiagnosis and overtreatment has been discussed in a number of posts on this site. And back in
The problem of overdiagnosis and overtreatment has been discussed in a number of posts on this site. And back in  Thyroid gland. Credit: Mayo Foundation for Medical Education and Research
Thyroid gland. Credit: Mayo Foundation for Medical Education and Research