![]() The following research finds a link (it doesn't establish cause) - but these interesting associations with vitamin D keep popping up. The research looked at leukemia rates in 172 countries and found that living closer to the equator (and assumed to have higher levels of vitamin D due to sunlight exposure) is linked to lower levels of leukemia. By far the best source of vitamin D is sunshine (and not food). From Medical Xpress:
The following research finds a link (it doesn't establish cause) - but these interesting associations with vitamin D keep popping up. The research looked at leukemia rates in 172 countries and found that living closer to the equator (and assumed to have higher levels of vitamin D due to sunlight exposure) is linked to lower levels of leukemia. By far the best source of vitamin D is sunshine (and not food). From Medical Xpress:
Researchers link higher risk of leukemia to low sunlight and vitamin D
Epidemiologists at University of California, San Diego School of Medicine report that persons residing at higher latitudes, with lower sunlight/ultraviolet B (UVB) exposure and greater prevalence of vitamin D deficiency, are at least two times at greater risk of developing leukemia than equatorial populations.
These results suggest that much of the burden of leukemia worldwide is due to the epidemic of vitamin D deficiency we are experiencing in winter in populations distant from the equator," said Cedric Garland, DrPH, adjunct professor in the Department of Family Medicine and Public Health and member of Moores Cancer Center at UC San Diego Health. "People who live in areas with low solar ultraviolet B exposure tend to have low levels of vitamin D metabolites in their blood," Garland said. "These low levels place them at high risk of certain cancers, including leukemia."
According to the American Cancer Society, 54,270 cases and 24,450 deaths from leukemia occur in the United States alone each year. There is no known way to prevent most types of leukemia, though some types may be prevented by avoiding high doses of ionizing radiation, exposure to the chemical benzene, smoking and certain types of chemotherapy.
The UC San Diego study analyzed age-adjusted incidence rates of leukemia in 172 countries from GLOBOCAN, an international agency for research on cancer that is part of the World Health Organization, comparing that information with cloud cover data from the International Satellite Cloud Climatology Project. The study follows similar investigations by Garland and colleagues of other cancers, including breast, colon, pancreas, bladder and multiple myeloma. In each study, they found that reduced UVB radiation exposure and lower vitamin D levels were associated with higher risks of cancer.
Leukemia rates were highest in countries relatively closer to the poles, such as Australia, New Zealand, Chile, Ireland, Canada and the United States. They were lowest in countries closer to the equator, such as Bolivia, Samoa, Madagascar and Nigeria.

 Two recent studies found health problems associated with low levels of
Two recent studies found health problems associated with low levels of 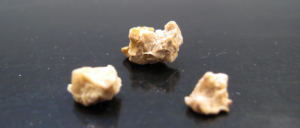 Once again, a study finds that foods are superior to supplements (here calcium supplements). It appears that eating foods rich in calcium has protective effects against kidney stones, but taking calcium supplements may result in kidney stone growth.
Once again, a study finds that foods are superior to supplements (here calcium supplements). It appears that eating foods rich in calcium has protective effects against kidney stones, but taking calcium supplements may result in kidney stone growth.
 Again, more benefits of vitamin D. Think of it as the
Again, more benefits of vitamin D. Think of it as the  The study results of 218 overweight, postmenopausal women who had insufficient levels of vitamin D (like most people) at the beginning of the study found that weight loss (including exercise), in combination with vitamin D supplementation, had a greater effect on reducing chronic inflammation than weight loss alone.
The study results of 218 overweight, postmenopausal women who had insufficient levels of vitamin D (like most people) at the beginning of the study found that weight loss (including exercise), in combination with vitamin D supplementation, had a greater effect on reducing chronic inflammation than weight loss alone.