 Gout is something that is not discussed that much, but it has been increasing in recent years and now afflicts about 3.9% of adults in the US. Gout is a form of inflammatory arthritis, characterized by recurrent attacks of pain, tenderness, and swelling of a joint, frequently the joint of the big toe. It is caused by elevated levels of uric acid in the blood (known as hyperuricaemia).
Gout is something that is not discussed that much, but it has been increasing in recent years and now afflicts about 3.9% of adults in the US. Gout is a form of inflammatory arthritis, characterized by recurrent attacks of pain, tenderness, and swelling of a joint, frequently the joint of the big toe. It is caused by elevated levels of uric acid in the blood (known as hyperuricaemia).
Gout occurs more commonly in men ages 40 and older, who eat a lot of meat and seafood, drink a lot of alcohol (especially beer) or sweetened drinks, have high blood pressure, metabolic syndrome, or are overweight. Gout used to be known as "the disease of kings" or "rich man's disease". [On the other hand, past research has shown that consumption of coffee, cherries, vitamin C foods, and dairy products, losing weight and physical fitness seems to decrease the risk.]
Recent research showed that the DASH diet reduces blood pressure and reduces uric acid in the blood, which is why a research team (study in The BMJ) now looked at whether it lowers the risk of gout. The Dietary Approaches to Stop Hypertension or DASH diet is high in fruit, vegetables, whole grains, legumes, nuts, and low-fat dairy, and low in red and processed meats, salt, and sugary drinks. On the other hand, the typical Western diet has higher intakes of red and processed meats, sweetened beverages, sweets, desserts, French fries, and refined grains. The researchers analysed data on a total of 44,444 male health professionals, who had no history of gout at the start of the study. During the 26 years of the observational study, they documented 1731 cases of gout.
The researchers found that eating a more DASH type diet - a diet rich in fruits, vegetables, legumes, nuts, whole grains, and low in salt, sugary drinks, and red and processed meats, is associated with a lower risk of gout. On the other hand, a more 'Western' diet is associated with a higher risk of gout. They found that the effects are dose dependent - the more DASH-type diet, the lower the risk of gout. Bottom line: Once again, eating lots of fruits, vegetables, nuts, legumes, and whole grains is linked to health benefits. From Science Daily:
Diet rich in fruit, vegetables and whole grains may lower risk of gout
A diet rich in fruit and vegetables, nuts and whole grains and low in salt, sugary drinks, and red and processed meats, is associated with a lower risk of gout, whereas a typical 'Western' diet is associated with a higher risk of gout, finds a study published by The BMJ.
Gout is a joint disease which causes extreme pain and swelling. It is most common in men aged 40 and older and is caused by excess uric acid in the blood (known as hyperuricaemia) which leads to uric acid crystals collecting around the joints. The Dietary Approaches to Stop Hypertension (DASH) diet reduces blood pressure and is recommended to prevent heart disease. It has also been found to lower uric acid levels in the blood. Therefore, the DASH diet may lower the risk of gout.
To investigate this further, a team of US and Canada based researchers examined the relationship between the DASH and Western dietary patterns and the risk of gout. They analysed data on over 44,000 men aged 40 to 75 years with no history of gout who completed detailed food questionnaires in 1986 that was updated every four years through to 2012.
Each participant was assigned a DASH score (reflecting high intake of fruits, vegetables, nuts and legumes, such as peas, beans and lentils, low-fat dairy products and whole grains, and low intake of salt, sweetened beverages, and red and processed meats) and a Western pattern score (reflecting higher intake of red and processed meats, French fries, refined grains, sweets and desserts). During 26 years of follow-up, a higher DASH score was associated with a lower risk for gout, while a higher Western pattern was associated with an increased risk for gout.
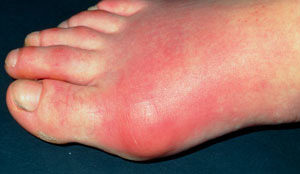
 Gout. Credit: NHS in the UK
Gout. Credit: NHS in the UK

 The research finding of so many baby foods with elevated arsenic levels (above the legal limit) in the European Union made me wonder about arsenic standards in baby cereals in the US. It turns out that the US has "parallel" standards to the European Union. The EU has "maximum 0.1 milligrams of arsenic per kilogram of rice" (this standard has been in place since January 2016), and in 2016 the US the FDA proposed a "maximum allowed standard of 100 ppb (parts per billion)" in infant rice cereal.
The research finding of so many baby foods with elevated arsenic levels (above the legal limit) in the European Union made me wonder about arsenic standards in baby cereals in the US. It turns out that the US has "parallel" standards to the European Union. The EU has "maximum 0.1 milligrams of arsenic per kilogram of rice" (this standard has been in place since January 2016), and in 2016 the US the FDA proposed a "maximum allowed standard of 100 ppb (parts per billion)" in infant rice cereal. An article was just published in a research journal to discuss the fact that humans - in part due to
An article was just published in a research journal to discuss the fact that humans - in part due to  This site has several
This site has several  Good news! Once again a study has confirmed that eating fresh fruits is associated with a lower incidence of type 2 diabetes. And even better - there is a dose related relationship - the more one eats daily, the better. So don't worry about the "sugar content" of fruit - the key is to eat fruit (as well as vegetables) to lower the risk of getting diabetes. And if you have type 2 diabetes, it will lower the incidence of death and complications from diabetes.
Good news! Once again a study has confirmed that eating fresh fruits is associated with a lower incidence of type 2 diabetes. And even better - there is a dose related relationship - the more one eats daily, the better. So don't worry about the "sugar content" of fruit - the key is to eat fruit (as well as vegetables) to lower the risk of getting diabetes. And if you have type 2 diabetes, it will lower the incidence of death and complications from diabetes. A recent study looking at high dose supplementation of vitamin D found that it did not prevent cardiovascular disease. This study came about because of earlier studies observing that there is a higher incidence of cardiovascular disease in persons with low vitamin D levels (as measured in their blood). But such results from observational studies need rigorous testing in studies where people are randomly assigned to groups, and that are "double-blind" (no one knows who is getting the vitamin D until the end of the study) to eliminate bias. And this is what was done in this study, with the result that monthly high doses of vitamin D3 for 3 years did not prevent cardiovascular disease (including stroke, heart attacks, hypertension, etc) - as seen in that there were no group differences between the vitamin D and placebo groups. Finding no effects are "
A recent study looking at high dose supplementation of vitamin D found that it did not prevent cardiovascular disease. This study came about because of earlier studies observing that there is a higher incidence of cardiovascular disease in persons with low vitamin D levels (as measured in their blood). But such results from observational studies need rigorous testing in studies where people are randomly assigned to groups, and that are "double-blind" (no one knows who is getting the vitamin D until the end of the study) to eliminate bias. And this is what was done in this study, with the result that monthly high doses of vitamin D3 for 3 years did not prevent cardiovascular disease (including stroke, heart attacks, hypertension, etc) - as seen in that there were no group differences between the vitamin D and placebo groups. Finding no effects are "