 Yikes! A good reason to lose weight now rather than years from now, and the importance of not ignoring a weight gain (you know, over the years as the pounds slowly creep up). The researchers found that for every 10 years of being overweight as an adult, there was an associated 7% increase in the risk for all obesity-related cancers. The degree of overweight (dose-response) during adulthood was important in the risk of developing cancer, especially for endometrial cancer. This study just looked at postmenopausal women, so it is unknown if it applies to men. From Medscape:
Yikes! A good reason to lose weight now rather than years from now, and the importance of not ignoring a weight gain (you know, over the years as the pounds slowly creep up). The researchers found that for every 10 years of being overweight as an adult, there was an associated 7% increase in the risk for all obesity-related cancers. The degree of overweight (dose-response) during adulthood was important in the risk of developing cancer, especially for endometrial cancer. This study just looked at postmenopausal women, so it is unknown if it applies to men. From Medscape:
Longer Duration of Overweight Increases Cancer Risk in Women
A longer duration of being overweight during adulthood significantly increased the incidence of all cancers that are associated with obesity, a new study in postmenopausal women has concluded. The large population-based study was published August 16 in PLoS Medicine.
Dr Arnold and colleagues found that for every 10 years of being overweight as an adult, there was an associated 7% increase in the risk for all obesity-related cancers. The risk was highest for endometrial cancer (17%) and kidney cancer (16%). For breast cancer, the increased risk was 5%, but no significant associations were found for rectal, liver, gallbladder, pancreatic, ovarian, and thyroid cancer.
When the authors took into account the degree of excess weight over time, the risks were further increased, and there were "clear dose-response relationships," they note. Again, the risk was highest for endometrial cancer. For each additional decade spent with a body mass index (BMI) that was 10 units above normal weight, there was a 37% increase in the risk for endometrial cancer.
Study Details: The researchers used data from the huge American Women's Health Initiative (WHI) trial of postmenopausal women (aged 50 to 79 years at time of study enrollment). For this analysis, the team focused on a cohort of 73,913 postmenopausal women. During a mean follow-up of 12.6 years, 6301 obesity-related cancers were diagnosed. About 40% (n = 29,770) of women in the cohort were never overweight during their adult life....Women who were ever overweight were on average overweight for about 30 years, while those who were ever obese had been so for an average of 20 years. The authors found that the risk of being diagnosed with an obesity-related cancer rose for every 10 years of being overweight.

 The problem of overdiagnosis and overtreatment has been discussed in a number of posts on this site. And back in
The problem of overdiagnosis and overtreatment has been discussed in a number of posts on this site. And back in  Get active, really active, to reduce your risk for 5 diseases: breast cancer, colon cancer, heart disease, and ischemic stroke. Instead of the 150 minutes of brisk walking or 75 minutes per week of running (which is equal to the 600 metabolic equivalent (MET) minutes now recommended by the World Health Organization), this study found that much more exercise is needed for
Get active, really active, to reduce your risk for 5 diseases: breast cancer, colon cancer, heart disease, and ischemic stroke. Instead of the 150 minutes of brisk walking or 75 minutes per week of running (which is equal to the 600 metabolic equivalent (MET) minutes now recommended by the World Health Organization), this study found that much more exercise is needed for 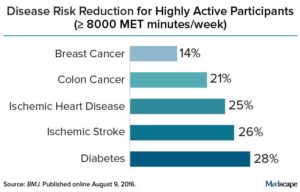 Credit: Medscape
Credit: Medscape Yup, according to a new mega-study, being overweight or obese is linked to higher risk of dying prematurely than being normal weight. And the more you weigh, the greater the risk.
Yup, according to a new mega-study, being overweight or obese is linked to higher risk of dying prematurely than being normal weight. And the more you weigh, the greater the risk. 
 Surprising study results. The question is why would having higher education somehow be associated with higher incidence of brain tumors? Is there something about sitting and studying, or sitting in an office for hours on end - perhaps next to something with high electromagnetic fields, that leads to this result? Or is it what a
Surprising study results. The question is why would having higher education somehow be associated with higher incidence of brain tumors? Is there something about sitting and studying, or sitting in an office for hours on end - perhaps next to something with high electromagnetic fields, that leads to this result? Or is it what a  A second study was just published about the benefits of eating whole grains daily - again a significantly lower risk of premature death, and again the effects were dose-related. That is, the more whole grains eaten daily, the lower the risk of early death. Like the
A second study was just published about the benefits of eating whole grains daily - again a significantly lower risk of premature death, and again the effects were dose-related. That is, the more whole grains eaten daily, the lower the risk of early death. Like the