 Get active, really active, to reduce your risk for 5 diseases: breast cancer, colon cancer, heart disease, and ischemic stroke. Instead of the 150 minutes of brisk walking or 75 minutes per week of running (which is equal to the 600 metabolic equivalent (MET) minutes now recommended by the World Health Organization), this study found that much more exercise is needed for best health results.
Get active, really active, to reduce your risk for 5 diseases: breast cancer, colon cancer, heart disease, and ischemic stroke. Instead of the 150 minutes of brisk walking or 75 minutes per week of running (which is equal to the 600 metabolic equivalent (MET) minutes now recommended by the World Health Organization), this study found that much more exercise is needed for best health results.
This study (which was a review and analysis of 174 studies) found that there is a dose-response effect, with the most reduction in the risk of the 5 conditions by getting 3000 to 4000 MET minutes per week. This sounds like a lot, but the researchers point out that this can be achieved by incorporating exercise into your daily routines. The researchers write: "A person can achieve 3000 MET minutes/week by incorporating different types of physical activity into the daily routine—for example, climbing stairs 10 minutes, vacuuming 15 minutes, gardening 20 minutes, running 20 minutes, and walking or cycling for transportation 25 minutes on a daily basis would together achieve about 3000 MET minutes a week."
So start thinking creatively about how to increase exercise or activity into your daily life, especially moderate or vigorous intensity activity. For example, park your car far from the store door, or better yet, bicycle or walk to the store from home. From Medscape:
Get Moving: High Physical-Activity Level Reduces Risk of 5 Diseases
High levels of physical activity can reduce the risk for five major diseases, including type 2 diabetes, new research shows. Findings from the systematic review and meta-analysis were published online ....The data, from a total 174 studies comprising 149,184,285 total person-years of follow-up, suggest that the more total regular daily physical activity one engages in — including recreation, transportation, occupational activity, and/or daily chores — the lower the risks for breast cancer, colon cancer, diabetes, ischemic heart disease, and ischemic stroke.
However, significant reductions in those conditions were seen only with total activity levels considerably higher than the minimum 600 metabolic equivalent (MET) minutes per week recommended by the World Health Organization for health benefits. That 600 METs equates to about 150 minutes/week of brisk walking or 75 minutes/week of running. (A MET is defined as the ratio of the metabolic rate during that activity to the metabolic rate when resting.) Risks of the five conditions dropped significantly with an increase in MET minutes per week from 600 to 3000 to 4000, with less additive benefit seen above that level.
For reference, the authors say, "a person can achieve 3000 MET minutes/week by incorporating different types of physical activity into the daily routine — for example, climbing stairs 10 minutes, vacuuming 15 minutes, gardening 20 minutes, running 20 minutes, and walking or cycling for transportation 25 minutes on a daily basis would together achieve about 3000 MET minutes a week." "This amount might seem a bit large, but this is about total activity across all domains of life.…For people who currently don't exercise, clinicians could encourage them to incorporate physical activity into their daily routines, [such as] turning household chores into exercise.
Another recent meta-analysis of trials involving more than one million individuals indicated that an hour of moderate-intensity activity, such as brisk walking or cycling, offsets the health risks of 8 hours of sitting. The message that physical inactivity is a killer — leading to 5.3 million premature deaths annually worldwide, which is as many as caused by smoking and twice as many as associated with obesity, has been emerging over the past few years, with warnings that "sitting is the new smoking."
This new research is the first meta-analysis to quantify the dose-response association between total physical activity across all domains and the risk of five chronic diseases. The 174 prospective cohort studies included 35 for breast cancer, 19 for colon cancer, 55 for diabetes, 43 for ischemic heart disease, and 26 for ischemic stroke. (Some included more than one end point.)....Higher levels of total physical activity were associated with lower risks of all five outcomes.
With the development of diabetes, for example, compared with no physical activity, those with 600 MET minutes per week (the minimum recommended level of activity) had a 2% lower risk. That risk reduction jumped by an additional 19% with an increase from 600 to 3600 METs/week. Gains were smaller above that, with the increase of total activity from 9000 to 12,000 MET minutes/week yielding only an additional 0.6% diabetes reduction.
Overall, compared with insufficiently active individuals (total activity < 600 MET minutes/week), the risk reduction for those in the highly active category (≥ 8000 MET minutes/week) was 14% for breast cancer; 21% for colon cancer; 28% for diabetes; 25% for ischemic heart disease; and 26% for ischemic stroke.
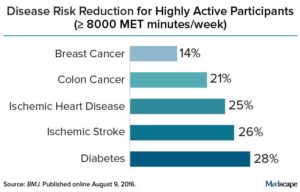 Credit: Medscape
Credit: Medscape
 There is growing evidence that the presence of certain species of bacteria in the gut microbiome are associated with a higher stroke risk, while other bacteria are associated with a lower risk and health. Two recent studies went further and found that the presence (or higher levels) of certain bacteria are associated with severe ischemic strokes and a poorer recovery.
There is growing evidence that the presence of certain species of bacteria in the gut microbiome are associated with a higher stroke risk, while other bacteria are associated with a lower risk and health. Two recent studies went further and found that the presence (or higher levels) of certain bacteria are associated with severe ischemic strokes and a poorer recovery. To improve your gut microbes and lower stroke risk: most important is to improve your diet (eat a healthy diet rich in fruits, vegetables, whole grains, nuts, seeds, legumes, some fermented foods, and try to avoid highly processed foods). Also, good for gut microbes: increase your physical activity or amounts of exercise, don't smoke, and try to maintain a healthy weight. Another option is getting a fecal microbial transplant.
To improve your gut microbes and lower stroke risk: most important is to improve your diet (eat a healthy diet rich in fruits, vegetables, whole grains, nuts, seeds, legumes, some fermented foods, and try to avoid highly processed foods). Also, good for gut microbes: increase your physical activity or amounts of exercise, don't smoke, and try to maintain a healthy weight. Another option is getting a fecal microbial transplant.
 Once again a study found health benefits from eating a diet rich in plant-based foods, such as vegetables, fruits, whole grains, legumes, beans, nuts, and seeds This time the health benefit was a lower incidence of stroke.
Once again a study found health benefits from eating a diet rich in plant-based foods, such as vegetables, fruits, whole grains, legumes, beans, nuts, and seeds This time the health benefit was a lower incidence of stroke. Very interesting - that infections may be a trigger for a coronary heart disease event such as heart attack or ischemic stroke, within the next 3 months. [Ischemic strokes are strokes caused by a blood clot.]
Very interesting - that infections may be a trigger for a coronary heart disease event such as heart attack or ischemic stroke, within the next 3 months. [Ischemic strokes are strokes caused by a blood clot.]  Study after study finds negative health effects from air pollution, such as heart disease (
Study after study finds negative health effects from air pollution, such as heart disease ( Uh oh - once again a drug taken for a common problem (heartburn) is linked to an unexpected negative health effect (higher risk of strokes). Millions of Americans take proton pump inhibitors (PPIs) to treat acid reflux and heartburn. They are among the most prescribed drugs in the United States, are frequently taken for long periods of time, and are available over the counter. But according to preliminary research presented at a 2016 American Heart Association conference, these medications may also increase the risk of ischemic stroke. Ischemic strokes, which are the most common type of stroke, occur when a blood clot cuts off blood flow to the brain.
Uh oh - once again a drug taken for a common problem (heartburn) is linked to an unexpected negative health effect (higher risk of strokes). Millions of Americans take proton pump inhibitors (PPIs) to treat acid reflux and heartburn. They are among the most prescribed drugs in the United States, are frequently taken for long periods of time, and are available over the counter. But according to preliminary research presented at a 2016 American Heart Association conference, these medications may also increase the risk of ischemic stroke. Ischemic strokes, which are the most common type of stroke, occur when a blood clot cuts off blood flow to the brain. Get active, really active, to reduce your risk for 5 diseases: breast cancer, colon cancer, heart disease, and ischemic stroke. Instead of the 150 minutes of brisk walking or 75 minutes per week of running (which is equal to the 600 metabolic equivalent (MET) minutes now recommended by the World Health Organization), this study found that much more exercise is needed for
Get active, really active, to reduce your risk for 5 diseases: breast cancer, colon cancer, heart disease, and ischemic stroke. Instead of the 150 minutes of brisk walking or 75 minutes per week of running (which is equal to the 600 metabolic equivalent (MET) minutes now recommended by the World Health Organization), this study found that much more exercise is needed for  Credit: Medscape
Credit: Medscape Another study that found benefits to dog ownership. The study authors concluded that: "Our study provides evidence that dog owners are at a lower risk for ischemic stroke, hemorrhagic stroke and heart failure." This could be to daily exercise, or that dog ownership results in less stress or better psychosocial health, or even some other reason (perhaps dog owners are healthier to start with). Note: myocardial infarction (MI) is commonly known as a heart attack. From Medscape:
Another study that found benefits to dog ownership. The study authors concluded that: "Our study provides evidence that dog owners are at a lower risk for ischemic stroke, hemorrhagic stroke and heart failure." This could be to daily exercise, or that dog ownership results in less stress or better psychosocial health, or even some other reason (perhaps dog owners are healthier to start with). Note: myocardial infarction (MI) is commonly known as a heart attack. From Medscape: