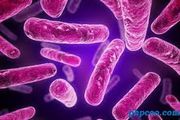
 Today I read an interesting article about bacterial vaginosis and research on bacteria that could finally treat it effectively. Bacterial vaginosis (BV) appears to be a problem with the microbial community of a woman's vagina being out of whack (dysbiosis). Common symptoms include increased white or gray vaginal discharge that often smells like fish, there may be burning with urination and sometimes itching, and the discharge has higher than normal vaginal pH (alkaline).
Today I read an interesting article about bacterial vaginosis and research on bacteria that could finally treat it effectively. Bacterial vaginosis (BV) appears to be a problem with the microbial community of a woman's vagina being out of whack (dysbiosis). Common symptoms include increased white or gray vaginal discharge that often smells like fish, there may be burning with urination and sometimes itching, and the discharge has higher than normal vaginal pH (alkaline).
One bacteria that seems to be very important and beneficial for vaginal health is Lactobacillus crispatus. Research suggests that L. crispatus may be a treatment for both bacterial vaginosis and urinary tract infections. Currently the treatment for BV is a course of antibiotics, but the problem recurs frequently.
In the US, the vaginal product Lactin-V (containing the freeze dried human vaginal strain of L. crispatus CTV-05, and used as an vaginal suppository) is currently being tested (with so far positive results in phase 2 clinical trials) for both bacterial vaginosis and recurrent urinary tract infections (UTIs). But it may be years away from FDA approval. The biopharmaceutical company Osel Inc. is currently conducting research on this product, and as of May 2016 is recruiting women for a phase 2b clinical study of this product in the US.
Other sources that I know of for the bacteria L. crispatus are: the probiotic Ordesa DonnaPlus+Intimate Flora (manufactured in Spain) and NaturaMedicatrix LactoGyn Crispatus Bio (made in Luxembourg). However, these are different strains of L. crispatus than what has been successfully tested using Lactin-V. (It is unknown whether this makes a difference.) Both are meant to be taken orally (swallowed daily) - which may or may not be an effective way to get L. crispatus in the vagina (it is unknown which way works best).
Other probiotics, especially Lactobacillus species, may also benefit vaginal health. One way to get an idea of products women find helpful is to look at user comments after products listed on Amazon. (By the way - douches, sprays, wipes, deodorizers, and special soaps will not help bacterial vaginosis.... Not at all.).
The following article was written by science journalist Kendall Powell. Do click on the link and read the entire article to get an idea of the complexity of the problem, the role of various bacteria in vaginal health, other health problems that occur with BV, ethnic differences, and how certain bacteria can alter vaginal mucus (leaving women vulnerable to infection). It is clear that much is unknown, but it looks like vaginal health depends on a "healthy microbial community". Excerpts from Mosaic:
The superhero in your vagina
The aisle is marked with a little red sign that says “Feminine Treatments”. Squeezed between the urinary incontinence pads and treatments for yeast infections, there is a wall of bottles and packages in every pastel shade imaginable. Feminine deodorant sprays, freshening wipes, washes for your “intimate area”.
Vaginal odor might be the last taboo for the modern woman.....The companies behind these products know that many women are looking for ways to counter embarrassing and debilitating symptoms such as vaginal odor and discharge. The culprit is often bacterial vaginosis, the most common vaginal infection you’ve probably never heard of. Nearly one-third of US women of reproductive age have it at any given time. The sad truth is that these sprays, soaps and wipes will not fix the problem. They will – in many cases – actually make it worse.
But while women try to mask embarrassing smells, a more sinister truth also remains under cover: the bacteria responsible are putting millions of women, and their unborn babies, at risk from serious health problems. All of which is making researchers look anew at the most private part of a woman’s body, to understand what it means to have a healthy – some prefer “optimal” – vagina and why that is so important for wider health.
Compared with those of other mammals, the human vagina is unique. As warm, moist canals exposed to all sorts of things including penises, babies and dirt, most mammalian vaginas harbour a diverse mix of bacteria. However, for many women, one or another species of Lactobacillus has become the dominant bacterial resident. Lactobacillus bacteria pump out lactic acid, which keeps the vaginal environment at a low, acidic pH that kills or discourages other bacteria, yeast and viruses from thriving. There are even hints that certain Lactobacillus species reinforce the mucus in the vagina that acts as a natural barrier to invaders.
For the most part, we’ve been happily cohabitating ever since, but it’s a delicate balancing act. Normal intrusions to the vaginal environment, such as semen (which causes vaginal pH to rise) or menstruation, can reduce numbers of Lactobacillus and allow other microbes, including those associated with bacterial vaginosis (BV), to flourish.
Her doctor explained that BV is a disturbance of the natural balance of bacteria that live inside the vagina. Sex with someone new, having multiple partners, and douching – rinsing out the vagina with a bag or bottle of liquid – can all contribute to getting BV, but it is not classified as a sexually transmitted disease. Mostly, how a woman develops BV is still a big mystery.
And if the embarrassment and discomfort weren’t enough, BV has a far more menacing side. Women affected have a higher risk of contracting sexually transmitted infections (STIs) like gonorrhoea and chlamydia, acquiring and transmitting HIV, and having pelvic inflammatory disease (which can lead to infertility) and other vaginal and uterine infections. During pregnancy, BV gives a woman a greater chance of having a preterm birth or passing infections to her baby, both of which can lead to lifelong problems for the baby.
Holmes felt the syndrome should be renamed bacterial vaginosis, which loosely translates to “too much bacteria”. And fulfilling three of the four Amsel criteria – thin vaginal discharge, vaginal pH greater than 4.5, positive whiff test and clue cells – is still used by many doctors today to diagnose BV.
They are realising that all Lactobacillus bacteria – long thought to keep vaginas healthy – are not created equal. For some researchers, L. crispatus is emerging as the vagina’s superhero. It not only pumps out the best mix of two different types of lactic acid to keep the vagina inhospitable to other bugs, but it also fortifies a woman’s vaginal mucus to trap and keep at bay HIV and other pathogens.
In 2011, Larry Forney, an evolutionary ecologist at University of Idaho in Moscow, and Jacques Ravel, a microbial genomicist from the University of Maryland School of Medicine in Baltimore, sequenced the bacterial species found in the vaginas of nearly 400 North American women who didn’t have the symptoms of BV. They found five different types of bacterial community. Four of these were dominated by different Lactobacillus species, but the fifth contained a diverse mix of microbes (including Gardnerella, Sneathia, Eggerthella and Mobiluncus species), many of which have been associated with BV.
The African studies leave researchers clamouring for better solutions for these women. Like others, van de Wijgert believes that the solution lies in getting the right bacteria to set up house in women’s vaginas. In 2014, she found that Rwandan sex workers with L. crispatus dominant in their vaginas were less likely to have HIV and other STIs. This bacterium may have even protected the clients of HIV-positive sex workers somewhat, because these women were also less likely to shed HIV in the vagina.
 Lactobacillus crispatus Credit: MicrobeWiki
Lactobacillus crispatus Credit: MicrobeWiki
 A group of international researchers got together and proposed reclassifying all the Lactobacillus species into 25 different groups (genera) a few years ago.
A group of international researchers got together and proposed reclassifying all the Lactobacillus species into 25 different groups (genera) a few years ago.
 Over the years I've received many questions about vegan versus kimchi that contains seafood. Are the microbes in the kimchi the same?
Over the years I've received many questions about vegan versus kimchi that contains seafood. Are the microbes in the kimchi the same?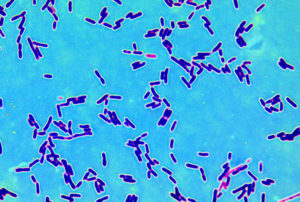
 Is the Mediterranean style diet the future in breast cancer prevention? The following study was done in primates, but it makes sense that the results would also be true for humans: that the type of diet eaten influences the breast microbiome. This means the community of microbes that live in the breast. Yes, it's true - studies show that there is a breast microbiome and it varies between those who have breast cancer and those who don't (healthy breasts).
Is the Mediterranean style diet the future in breast cancer prevention? The following study was done in primates, but it makes sense that the results would also be true for humans: that the type of diet eaten influences the breast microbiome. This means the community of microbes that live in the breast. Yes, it's true - studies show that there is a breast microbiome and it varies between those who have breast cancer and those who don't (healthy breasts). Today I read an interesting article about bacterial vaginosis and research on bacteria that could finally treat it effectively. Bacterial vaginosis (BV) appears to be a problem with the microbial community of a woman's vagina being out of whack (dysbiosis). Common symptoms include increased white or gray vaginal discharge that often smells like fish, there may be burning with urination and sometimes itching, and the discharge has higher than normal vaginal pH (alkaline).
Today I read an interesting article about bacterial vaginosis and research on bacteria that could finally treat it effectively. Bacterial vaginosis (BV) appears to be a problem with the microbial community of a woman's vagina being out of whack (dysbiosis). Common symptoms include increased white or gray vaginal discharge that often smells like fish, there may be burning with urination and sometimes itching, and the discharge has higher than normal vaginal pH (alkaline).