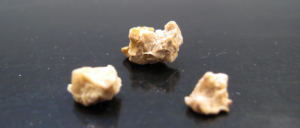
Finally, a study was done examining whether the kidneys have a microbiome (community of fungi, viruses, and bacteria). The answer is yes, the kidneys have a microbiome and the composition of the microbes plays a role in kidney health and whether a person develops kidney stones or not. This makes sense - all our other organs have microbiomes.
This multi-part study showed that the urinary tract is not sterile, and that low levels of bacteria are normal. Additionally, they found that the presence of the beneficial bacteria L. crispatus is found in the absence of kidney stones, while E.coli is associated with the development of kidney stones. (Interestingly, L. crispatus is also found in the healthy vagina and can treat bacterial vaginosis.)
The researchers found that the L. crispatus somehow blocked E.coli's ability to form kidney stones.
Antibiotic use was associated with bacteria that promoted the development of kidney stones because antibiotics kill off Lactobacillus species and promote the growth of kidney stone forming species (e.g., E. coli). Other studies also find that bacteria such as E.coli (as well as Proteus and Klebsiella) are frequently associated with UTIs, kidney stone formation, and kidney infection (pyelonephritis).
From Medical Xpress: First full characterization of kidney microbiome unlocks potential to prevent kidney stones
Cleveland Clinic researchers have found definitive proof of a kidney microbiome that influences renal health and kidney stone formation, demonstrating that the urinary tract is not sterile and low levels of bacteria are normal. ...continue reading "Bacteria In The Kidney Microbiome Can Prevent Or Promote Kidney Stones"


 The study was done in mice with persistent Lyme disease, but the results also (probably) apply to humans with persistent Lyme disease infections. None of the single antibiotics completely eradicated the bacteria, but the following 4 dual combinations were effective: doxycycline + ceftriaxone, dapsone + rifampicin, dapsone + clofazimine, doxycycline + cefotaxime. Also effective were 3 triple antibiotic combinations: doxycycline + ceftriaxone+ carbomycin, doxycycline + cefotaxime+ loratadine, dapsone+ rifampicin+ clofazimine. The drugs were given for 28 days two months after infection.
The study was done in mice with persistent Lyme disease, but the results also (probably) apply to humans with persistent Lyme disease infections. None of the single antibiotics completely eradicated the bacteria, but the following 4 dual combinations were effective: doxycycline + ceftriaxone, dapsone + rifampicin, dapsone + clofazimine, doxycycline + cefotaxime. Also effective were 3 triple antibiotic combinations: doxycycline + ceftriaxone+ carbomycin, doxycycline + cefotaxime+ loratadine, dapsone+ rifampicin+ clofazimine. The drugs were given for 28 days two months after infection.
 Fermented foods include: yogurt, buttermilk, sour cream, cheese, kefir, fermented vegetables, kimchi, natto, miso, sauerkraut, traditional pickles, traditional sourdough bread, apple cider vinegar, and kombucha. To quickly improve the gut microbiome, try to eat six 1/2 cup servings each day for a
Fermented foods include: yogurt, buttermilk, sour cream, cheese, kefir, fermented vegetables, kimchi, natto, miso, sauerkraut, traditional pickles, traditional sourdough bread, apple cider vinegar, and kombucha. To quickly improve the gut microbiome, try to eat six 1/2 cup servings each day for a  Well, the following findings make total sense. A recent
Well, the following findings make total sense. A recent  The issue of
The issue of