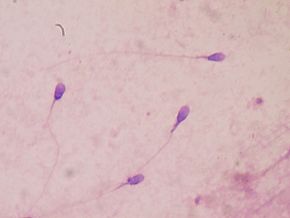
 Two years ago scientists reported an alarming and steep decline in sperm counts in men from Western industrialized countries over the last 40 years. Both sperm count and sperm concentration declined 50 to 60% in this period in men in North America, Europe, Australia, and New Zealand. Especially concerning was that there was no evidence of this year by year decline leveling off.
Two years ago scientists reported an alarming and steep decline in sperm counts in men from Western industrialized countries over the last 40 years. Both sperm count and sperm concentration declined 50 to 60% in this period in men in North America, Europe, Australia, and New Zealand. Especially concerning was that there was no evidence of this year by year decline leveling off.
What does this mean? As these declines continue, more and more men will have sperm counts below the point at which they can reproduce. Instead they will be infertile or "sub-fertile" (fertilization is unlikely). According to the World Health Organization (WHO), a sperm count of below 15 million per ml makes a man subfertile. However, also of concern is the threshold level associated with a "decreased monthly probability of conception", which is 40 million/ml - which means conception will take significantly longer (due to impaired ability to fertilize an egg).
A recent Univ. of Geneva study looked at semen quality of 2523 young men (aged 18 to 22 years old) who were being drafted into the military in Switzerland. They found that average sperm quality and sperm concentration of the men, who were from all regions of Switzerland, was among the lowest in Europe (along with Germany, Denmark, and Norway).
In Europe, median sperm count ranges from 41 to 67 million per milliliter (ml), depending on the country. The researchers found that the group of Swiss men had a median sperm count of 48 million per ml. And 17 percent of the men had sperm counts below 15 million per ml (thus subfertile). By the way, countries with lower sperm counts and quality, have higher rates of testicular cancer - they go hand in hand.
Also, in a quarter of the Swiss men studied, less than 40 percent of sperm cells were motile (moved normally), and 43 percent of men had less than 4 percent normally formed sperm. Overall, only 38 percent of Swiss men had healthy sperm - that is, with concentration, motility, and morphology (shape, form) that met the WHO’s criteria for healthy sperm.
Why is this happening? The researchers found that of the men with very low sperm concentration, more of their mothers smoked during the pregnancy, which means there could be changes during embryonic development. Also, while this study did not discuss this, many other researchers say that sperm health is "the canary in the mine" for male health - evidence of harm to men from environmental and lifestyle influences.
These Western developed countries are awash in chemicals and plastics, also with endocrine disruptors (hormone disruptors) in our foods, our personal care products, in products all around us - and so studies find these chemicals in all of us (in varying degrees). Same with flame retardants, pesticides, "scented" products. Exposure to all sorts of environmental pollutants - whether in air, water, soil, our food - such as high levels of aluminum. All of these can have an effect on sperm counts and reproductive health. You can't totally avoid these chemicals, but you can try to lower your amounts of exposure (some tips to lower exposures).
From Medical Xpress: Poor semen quality in Switzerland ...continue reading "Male Fertility Is Plunging In Switzerland"
 Good news for those wondering if home births are as safe as hospital births. An international study says the answer is YES, for low-risk women who begin labor intending to give birth at home as compared to low-risk women intending to give birth in a hospital. Canadian researchers analyzed data from 14 international studies (including about 500,000 women planning on home births). A midwife was present at each birth. The risk of perinatal or neonatal death was not different when birth was intended at home or in hospital. The researchers defined perinatal death as stillbirth after labor starts through day 7 after birth. Neonatal death is defined as death after birth of a live baby from day 0 through day 28.
Good news for those wondering if home births are as safe as hospital births. An international study says the answer is YES, for low-risk women who begin labor intending to give birth at home as compared to low-risk women intending to give birth in a hospital. Canadian researchers analyzed data from 14 international studies (including about 500,000 women planning on home births). A midwife was present at each birth. The risk of perinatal or neonatal death was not different when birth was intended at home or in hospital. The researchers defined perinatal death as stillbirth after labor starts through day 7 after birth. Neonatal death is defined as death after birth of a live baby from day 0 through day 28.
 Two years ago
Two years ago  For a few years I've been noticing that studies of vitamin D have had mixed results for a number of medical conditions. A number of times
For a few years I've been noticing that studies of vitamin D have had mixed results for a number of medical conditions. A number of times  Many of us have concerns over the fact that people are constantly exposed to endocrine disruptors (chemicals that disrupt hormonal systems) in many common household and personal products. Even the vinyl flooring found in many homes contains phthalates, which are endocrine disrupting chemicals.
Many of us have concerns over the fact that people are constantly exposed to endocrine disruptors (chemicals that disrupt hormonal systems) in many common household and personal products. Even the vinyl flooring found in many homes contains phthalates, which are endocrine disrupting chemicals. Researchers have known for a while that human breast milk contains hundreds of
Researchers have known for a while that human breast milk contains hundreds of  Today's topic: BIRTH. Two recent studies have results that question some current medical practices, which are when to cut the umbilical cord, and hospital vs home birth differences in the baby's gut microbes.
Today's topic: BIRTH. Two recent studies have results that question some current medical practices, which are when to cut the umbilical cord, and hospital vs home birth differences in the baby's gut microbes. The following is a really nice article about endocrine disruptors (chemicals that can interfere with the body's hormonal system). Journalist Hillary Brueck writes about where they are found (all around us!), some of the many negative health effects, and about NYU physician and researcher
The following is a really nice article about endocrine disruptors (chemicals that can interfere with the body's hormonal system). Journalist Hillary Brueck writes about where they are found (all around us!), some of the many negative health effects, and about NYU physician and researcher  Pregnant women have been advised to keep their consumption of coffee and other caffeinated beverages (tea, sodas, cocoa, energy drinks), and chocolate containing foods to a minimum for decades. Currently the American College of Obstetrics recommends that women consume less than 200 mg of caffeine (from any source) per day during pregnancy. This is less than 2 cups of regular coffee or 4 cups of regular black tea. But a recent study's findings suggest that the levels should be kept much lower.
Pregnant women have been advised to keep their consumption of coffee and other caffeinated beverages (tea, sodas, cocoa, energy drinks), and chocolate containing foods to a minimum for decades. Currently the American College of Obstetrics recommends that women consume less than 200 mg of caffeine (from any source) per day during pregnancy. This is less than 2 cups of regular coffee or 4 cups of regular black tea. But a recent study's findings suggest that the levels should be kept much lower.